Regenerative Medicine For TB/SCI

This technology of Regenerative Medicine, known as Tissue Nanotransfection (TNT), has the potential to save and improve many lives. Victims of car crash and even deployed soldiers injured on the battle field suffering from Traumatic Brain or Spinal Cord Injuries. It’s a dime-sized silicone chip that “injects genetic code into skin cells. Turning those skin cells into other types of cells required for treating diseased conditions.”
It takes just a fraction of a second to simply touch the chip to the wounded area and then remove it. At that point, the cell reprogramming begins. According to Chandan Sen, PhD, director of the Center for Regenerative Medicine and Cell-Based Therapies at The Ohio State University Wexner Medical Center.
Lab Testing
In a series of lab tests, Regenerative Medicine researchers applied the chip to the injured legs of mice. Their vascular scans showed had little to no blood flow. “We reprogrammed their skin cells to become vascular cells,” Sen said. “Within a week we began noticing the transformation.”
By the second week, active blood vessels had formed through the use of TNT Regenerative Medicine. By the third week, the legs of the mice were saved—with no other form of treatment.
It extends the concept known as Regenerative Medicine gene therapy, and it has been around for quite some time. According to study collaborator James Lee, PhD, a professor of chemical and biomolecular engineering at Ohio State. The difference with this technology is how the DNA is delivered into the cells.
The chip, loaded with specific genetic code or certain proteins, is placed on the skin.Then a small electrical current creates channels in the tissue. The DNA or RNA is injected into those channels where it takes root and begins to reprogram the cells.
In a new study published in Nature Nanotechnology, first author Daniel Gallego-Perez of Ohio State demonstrated that the technique worked with up to 98 percent efficiently.
Future Prospects
What’s even more exciting is that this Regenerative Medicine not only works on the skin, but on any type of tissue. During the researchers they were able to grow brain cells on the skin surface of a mouse. Harvest them and then inject them into the mouse’s injured brain. Just a few weeks after having a stroke, brain function in the mouse was restored, and it was healed.
This technology does not require a laboratory or hospital and can actually be executed in the field. It’s less than 100 grams to carry and will have a long shelf life.
This Regenerative Medicine approach is currently awaiting FDA approval. Sen, who has been working on this for four years, expects TNT will be tested on humans within the year. He says he’s talking with Walter Reed National Medical Center now.
“We are proposing the use of skin as an agricultural land where you can essentially grow any cell of interest,” Sen said.
Because the technique uses a patient’s own cells and does not rely on medication. The Regenerative Medicine researchers expect it to be approved for human trials within a year.
The horizon for utilization of TNT Regenerative Medicine encompasses the ability to repair, supplement and replace any damaged part of the human body without invasive surgical procedures. The severed or damaged nerves occurring when someone suffers a Spinal Cord Injury can be repaired within several weeks. Restoring full functioning to wheel chair and bed ridden patients.
Patients that have had Traumatic Brain Injuries will now be able to benefit from TNT Regenerative Medicine in a dramatic fashion. Their own brain cells regenerated to replace the damaged areas without the concern of rejection from their system. This allows patients to go forward leading a normal life again and not even worry about taking anti-rejection medication for the rest of their life.
Sources:
Ohio State University – https://news.osu.edu/news/2017/08/07/regenerative-med-study/
Nature Nanotechnology _ http://www.nature.com/nnano/index.html?foxtrotcallback=true
Brain & S C Injury Home Repairs

Brain injury and/or Spinal Cord injury patients frequently require home revisions and repairs. When they are initially released from the hospital usually their primary residence has physical obstacles. Additionally, as time goes on, frequent changes will have to occur in their environment as their abilities and needs evolve.
VID_20160418_101134
Brain injury or spinal cord injury patient living in a place with stairs will need a ramp for ease of access. The ramp structure must meet local codes to allow ease of entry and exit from their residence. This is one of the types of assistance Carpenter’s Hands provides cost free for disadvantaged individuals residing in Jefferson County. This ministry is primarily comprised of Christian volunteers. They realize that they can not solve the major world issues on their own. However they can reach out and solve one individual’s problem. This approach ensures having a positive impact on someone’s life and well being. They only ask for a display of appreciation in the form of a Simple Smile and Thank You.
John Luther is the Director of Operations for Carpenter’s Hands. John is responsible to select, plan, schedule and execute all of the projects this organization schedules. He accompanies a team of volunteers, varying in composition depending on the day of the week and extent of the project. John remains to direct and assist them throughout the duration of the project to ensure its completion fulfills the needs of the client.

Brain Injury and Spinal Cord Injury Patients Ramps
I recently had the opportunity to spend some time with some members of the Carpenter’s Hands at one of their projects. They were constructing a ramp for an individual suffering from Parkinson. He required a cane plus walker to stabilize himself as he slowly moved around his home.
This client also suffers from Post Polio syndrome, which affects individuals who contracted Polio when they were young. When Post Polio individuals enter their late 50’s, their muscles begin to slowly weaken and break down. This makes it exceedingly difficult to utilize their legs as they age.
The combination of Parkinson with Post Polio means it is inevitable that he will shortly end up relying on a wheelchair to get around. This individual currently requires assistance from a friend or the fire department to get up and down his front steps. In the near future a wheelchair ramp will be a mandatory requirement with the proper sloping angle and turn around space.
Carpenter’s Hands plays a critical role in the everyday quality of life for an individual in need. Irrespective of their financial ability to afford the needed building changes to their home.

Construction of the Entry landing with sufficient room to accommodate a wheelchair and helper.
Adding the ramp with a slope so it can effectively handle a wheelchair

Reinforcing the ramp structure to stabilize and allow the addition of rails
Once the ramping is completed, the rails are pickup from a cabinet shop that donates them to the ministry. This organization relies on volunteers to build the projects from the community. They do need monetary donations and/or building materials to continue providing their services.
During a break in construction, one of the volunteers told me about a small project they initially undertook. This project evolved into something far more critical and extensive as they began working on it:
Carpenter’s Hands was contacted by a 99 year old woman, who was unable to close the front door of her home. When they arrived at her home, they saw that she was living in a Coal Miner’s Camp House. These were constructed in the late 1800’s in Mulga and Ensley, Alabama. The homes were a mass development of identical construction. Four rooms, with a fireplace in the center of the home to provide heating. She had been born in this home and lived her entire life here. The interior of the home was immaculate and her yard displayed the pride she took of maintaining the property.

Miner’s Home Mulga, Alabama
Due to her inability to close the door, she had backed the front room couch up to it. In an attempt to keep intruders out, she had been sleeping on that couch for the last couple of years.

Miner’s Home Camp Ensley, Alabama
Although she had lived in this well maintained property, she was concerned. There were elements in the area that gave her an uncomfortable feeling. As the team began to remove the siding around the door , they were confronted with extensive termite damage. They decided to determine the extent of the termite infestation and ended up exposing the entire front of the home. What they found was that the termites had eaten away the entire support structure except for two 2×4’s. So the roof was on the verge of collapsing down, which would totally demolish the home.
Carpenter’s Hands made a decision to delay the other projects currently on their schedule and completely rebuild the front of the home. To the individuals involved in this ministry the cost and physical labor were secondary considerations. When viewing the need of this one individual – a 99 year old woman living alone in the home she was born and raised in. As they expressed to me, ‘We know we can have very little impact on the major problems in the world, but we can have a positive impact on one person’s issues, so we try to solve one problem at a time.’
To contact: Carpenter’s Hands a ministry of Canterbury United Methodist Church
The Red Barn Equestrian Therapy

During 2016 we will be periodically blogging about resources, like The Red Barn Equestrian Therapy, listed on the site. Each location has been personally visited and we have had an opportunity to spend time viewing the facility plus discussing the services available. Traumatic Brain Injury Resources wants to provide the visitors to the site with some first hand insight on a wide variety of the resources listed throughout the state of Alabama.The information shared with you will be our impressions of their facilities, services available and the personnel I have met at each location.
You will be always able to just click on any resource listed and contact them directly to determine if they fit your situation and current needs. However, by offering you our perspective, when conducting a resource visitation, the additional depth of knowledge may be helpful in your decision making process.
This site will continue to monitor and add new resources, whenever we are aware of their existence and encourage visitors to notify us of any service providers they feel should be included.
 I recently visited The Red Barn meeting with the founder, Joy O’Neal, who spent the greater part of the day touring me through the facility while explaining the unique approach of equestrian therapy. Individuals in need of therapeutic intervention are often difficult to reach through the standard therapy programs available. The Red Barn has developed an equestrian therapy intervention program that breaks down those self imposed barriers. Here working one on one with a patient assisted by horses, allows them to introduce a series of training courses focused on improving their overall well being.
I recently visited The Red Barn meeting with the founder, Joy O’Neal, who spent the greater part of the day touring me through the facility while explaining the unique approach of equestrian therapy. Individuals in need of therapeutic intervention are often difficult to reach through the standard therapy programs available. The Red Barn has developed an equestrian therapy intervention program that breaks down those self imposed barriers. Here working one on one with a patient assisted by horses, allows them to introduce a series of training courses focused on improving their overall well being.

The Red Barn opened in 2009 with a profound faith in God’s Healing Hand to reach the injured through the utilization of equestrian therapy to lead them to a fuller and richer life while cooping with their afflictions. The approach here not only deals with the individual, but reaches out to encompass other family members to assist them in gaining a deeper understanding as to how they can effectively function as a total inclusive unit. This is reflected in the physical development of the 33 acres The Red Barn occupies and the staffs’ approach to every patient, analyzing his/her needs along with those of their family members.

As I toured the grounds, I was impressed with the degree of planning evidenced and the amount of development that had occurred to this property in a short period of time. It is evident that the personnel remains consistently focused on understanding the needs of patients and making the necessary adjustments to the facilities to meet those needs.
The Red Barn has a diverse staff focused on creating programs designed to enrich the training experience of the individuals participating while enhancing their growth. The full time staff’s expertise is further supplemented by a caring community of volunteers providing a wealth of knowledge and skills acquired in their professional careers.

During my visit I met with one of those individuals, Wyspr Black a CHA IRD certified instructor with a master’s from Auburn University in Rehabilitation Counseling and Vocational Education. Her special interest in working with individual’s suffering from traumatic brain injuries combined with her love of horses since she was eight, makes her an ideal fit for The Red Barn. Wyspr plays an instrumental role in developing and implementing equestrian therapy programs uniquely designed for Traumatic Brain Injury patients.

As evidenced in this photo, The Red Barn offers equestrian therapy and training for individuals with physical, cognitive and emotional disabilities teaching them life skills, which provide a solid foundation for developing a productive life. Depicted here is the initial teaching stall within the barn where a student begins to learn about the care and handling of a horse prior to meeting with a live animal. This organization offers an opportunity for individuals of all ages to explore and expand their horizons beyond the limitations experienced from Traumatic or Spinal Cord Injury.
The Red Barn has developed the following programs to serve this community’s needs:
THE RED BARN EQUESTRIAN THERAPY – SADDLE UP – Weekly riding lessons for those with physical, cognitive or emotional disabilities and special circumstances.

<
THE RED BARN EQUESTRIAN THERAPY – HORSE PLAY – Traditional day camps with art, music, outdoor education…and horses!

THE RED BARN EQUESTRIAN THERAPY – TAKE THE REINS – It is our honor and privilege to serve active or inactive military personnel. We offer a customized experience for each individual or group.
The Red Barn is a 501(c)3 agency relying on the contributions of the community to continue and expand the innovative work it does to develop effective rehabilitative programs for individuals with Traumatic Brain and Spinal Cord Injuries.
Source: http://www.theredbarn.org/
Neuronal Cells May be Repaired?
Neuronal cells may be repaired in the near future opening the potential to reverse brain damage, spinal cord injuries and the devastating effects of diseases such as MS, ALS, Parkinson’s, Dementia and Alzheimer. For the first time researchers have direct evidence that viruses can infect neuronal cells, raising hope that antiviral therapy might be effective against neurologic diseases and cell damage, according to a new study.
A neurological disorder is any disorder of the body nervous system. Structural, biochemical or electrical abnormalities in the brain, spinal cord or other nerves can result in a range of symptoms. Examples of symptoms include paralysis, muscle weakness, poor coordination, loss of mental control, sensation, seizures, confusion, pain and altered levels of consciousness
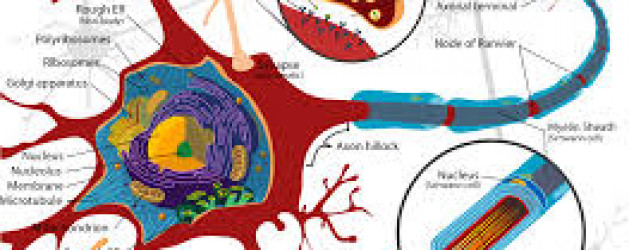
Neurons are nerve cells that transmit nerve signals to and from the brain at up to 200 mph. The neuron consists of a cell body (or soma) with branching dendrites (signal receivers) and a projection called an axon, which conduct the nerve signal. At the other end of the axon, the axon terminals transmit the electro-chemical signal across a synapse (the gap between the axon terminal and the receiving cell). The word “neuron” was coined by the German scientist Heinrich Wilhelm Gottfried von Waldeyer-Hartz in 1891 (he also coined the term “chromosome”).
There are different types of neuronal cells. They all carry electro-chemical nerve signals, but differ in structure (the number of processes, or axons, emanating from the cell body) and are found in different parts of the body.
- Sensory neurons or Bipolar neurons carry messages from the body’s sense receptors (eyes, ears, etc.) to the CNS. These neurons have two processes. Sensory neuron account for 0.9% of all neurons. (Examples are retinal cells, olfactory epithelium cells.)
- Motoneurons or Multipolar neurons carry signals from the CNS to the muscles and glands. These neurons have many processes originating from the cell body. Motoneurons account for 9% of all neurons. (Examples are spinal motor neurons, pyramidal neurons, Purkinje cells.)
- Interneurons or Pseudopolare (Spelling) cells form all the neural wiring within the CNS. These have two axons (instead of an axon and a dendrite). One axon communicates with the spinal cord; one with either the skin or muscle. These neurons have two processes. (Examples are dorsal root ganglia cells.)
The core component of the nervous system in general, and the brain in particular, is the neuron or nerve cell, the “brain cells” of popular language. A neuron is an electrically excitable cell that processes and transmits information by electro-chemical signalling. Unlike other cells, neurons never divide, and neither do they die off to be replaced by new ones. By the same token, they usually cannot be replaced after being lost, although there are a few exceptions.
Information transmission within the brain, such as takes place during the processes of memory encoding and retrieval, is achieved using a combination of chemicals and electricity. It is a very complex process involving a variety of interrelated steps, but a quick overview can be given here.
Unlike other body cells, most neurons in the human brain are only able to divide to make new cells (a process called neurogenesis) during fetal development and for a few months after birth.
These brain cells may increase in size until the age of about eighteen years, but they are essentially designed to last a lifetime.
During childhood, and particularly during adolescence, a process known as “synaptic pruning” occurs.
Although the brain continues to grow and develop, the overall number of neurons and synapses are reduced by up to 50%, removing unnecessary neuronal structures and allowing them to be replaced by more complex and efficient structures, more suited to the demands of adulthood.
The data demonstrate that Epstein Barr Virus (EBV) and Kaposi’s sarcoma–associated herpesvirus (KSHV) are able to effectively infect neuronal cell lines, as well as primary neurons. “This phenomenon may potentially provide clues to their contribution to the pathogenesis of human neural diseases,” stated the researchers, led by senior author Erle S. Robertson, PhD, of the University of Pennsylvania in Philadelphia, PA.
“In this study, for the first time, we have successfully demonstrated the in vitro infection of Sh-Sy5y (a human neuroblastoma cell line) and Ntera2 cells (a neuronally committed human teratocarcinoma cell line), as well as human primary neurons. We have also determined that the infection is predominately lytic. Additionally, we also report infection of neuronal cells by KSHV in vitro similar to that by EBV,” stated the authors.
They believe that these findings may “open new avenues of consideration related to neuronal pathologies and infection with these viruses. Furthermore, their contribution to chronic infection linked to neuronal disease will provide new clues to potential new therapies.”
In many debilitating neurodegenerative diseases, including MS, the efficiency of electrochemical signals is greatly reduced, they noted, often leading to problems related to cognition and muscular activity. “It is likely that viral infection with EBV or KSHV may severely reduce these signals, leading to reduced cognition and reduced neuromuscular function,” they stated.
The results clearly show that infection of neuronal cells can occur, but further studies are needed to understand the underlying mechanism of these infections and their relevance to neuronal diseases.
Sources:
http://www.neurologytimes.com/alzheimer-disease/herpes-viruses-infection-neurons#sthash.kOMeJYI8.dpuf
http://www.human-memory.net/brain_neurons.html
http://www.enchantedlearning.com/subjects/anatomy/brain/Neuron.shtml
Young Blood Rejuvenates Our Cells
IT SOUNDS like the dark plot of a vampire movie – Young blood rejuvenates our cells. In October 2014, people with Alzheimer’s disease started to be injected with the blood of young people in the hope that it will reverse some of the damage caused by that condition. But holds promise for individuals suffering for a wide range issues that have impacted their body and effected the quality of their life style. Just imagine the implications of reversing Traumatic Brain Injuries, Parkinson’s, MS, ALS, Repairing Damaged Organs, Surgical Healing, Aging of Skin, Muscle and Vascular Development.
In the first human trial of the effects of young blood, at Stanford University, infusions of blood plasma from young people are being given to older people. The preliminary results have surprised the research team, since it appears that young blood rejuvenates all of the cells within the recipients’ bodies are showing marked improvement.

Blood Stanford Test
The scientists behind the experiment have evidence on their side that young blood rejuvenates. Work in animals has shown that a transfusion of young mouse blood can improve cognition and the health of several organs in older mice. It could even make those animals look younger. The ramifications for the cosmetics and pharmaceutical industries could be huge, if the same thing happens in people.
The study was published in Nature Medicine in 2014. Immediately, emails flooded in to Wyss-Coray’s inbox. Alzheimer’s patients wanted infusions of young blood. So did numerous aged billionaires interested in the potential that young blood rejuvenates. One, who flies around in a jet with his name emblazoned on the side, invited Wyss-Coray to an Oscars after-party this year. (He didn’t go.) Another correspondent wrote with a more disturbing offer: he said he could provide blood from children of whatever age the scientists required. Wyss-Coray was appalled. “That was creepy,” he said.
But it wasn’t until spring 2012 that plans to form a company emerged. Nikolich, an entrepreneur and neuroscientist at Stanford, had flown to Hong Kong to visit the family of Chen Din-hwa, a Chinese billionaire known as the King of Cotton Yarn. Three years earlier, Chen had died, aged 89, with Alzheimer’s disease. His grandson told Nikolich that towards the end of his life, Chen barely recognised his own family. Then he had a plasma transfusion for an unrelated condition, which seemed to have a spectacular effect. His mind was clearer and he was suddenly cogent. His grandson indicated that Alzheimer’s disease seem to historical effect the male of the family often at an early age.
Nikolich told them about Wyss-Coray’s research and the potential for plasma-based therapies that revitalised the ageing brain. Before long, the conversation turned to starting a company. The family invested a year later. The money got Alkahest established and ready to launch the first human trial of young plasma.
Alkahest’s ultimate goal – to identify the key proteins in plasma that rejuvenate or age human tissues and then manufacture a product that uses them – could take 10 to 15 years. In the near term, the company has another strategy. Earlier this year, the Spanish blood products firm, Grifols, pledged $37.5m for a 45% stake in Alkahest. With another $12.5m, the company will bankroll more research in exchange for rights to Alkahest’s first products. Over the next two years, Alkahest will take human plasma and divide it into fractions that are rich in different proteins. Each fraction will then be tested in mice to see if they boost brain function. Any that do will be swiftly introduced into human trials and developed into the first generation of products.
The Alkahest trial is small. Sha, a specialist in behavioral neurology, can enroll only 18 people aged 50 to 90 with mild to moderate Alzheimer’s disease. Each receives a unit of young human plasma or saline once a week for four weeks. They have the next six weeks off, then have four more weeks of infusions. Those who had plasma first time around get saline and vice versa. The process is blinded, so neither the patients, nor their carers, nor Sha herself, know who is receiving what. Throughout the trial, doctors will look for cognitive improvements. Only at the end of the trial, as soon as October this year, will Sha analyse the findings.
If patients improve with infusions of young plasma, scientists will be ecstatic. But the finding, indicating that young blood rejuvenates, would need to be replicated, ideally at other hospitals, and in more patients, in order to convince researchers. If any benefits stand the test of time, the studies will move on, to tease out the best doses and ages at which to give plasma, how patients’ brains change, and whether improvements make a real difference to the life of someone who can no longer recognize their own family.
Then there is safety. Toying with the ageing process might backfire. Rando is concerned that pumping pro-youthful proteins into people for years could end up giving them cancer. Wyss-Coray agrees it is a worry, but points out that long-term growth hormone therapy appears to be safe. “We just don’t know yet whether or not it will be a problem,” he said.
Rando is more upbeat about infusing patients with pro-youthful proteins for short periods. An elderly person having surgery might get an infusion to help them heal like a teenager. “Let’s say it works. If you can target tissues and improve wound healing in older people, that would be a feasible approach. It would not be about making 90-year-olds younger, or having people live to 150. It’s about healthy living, not longer living,” he said.
In the first human trial of the effects of young blood, at Stanford University, infusions of blood plasma from young people are being given to older people. The preliminary results have surprised the research team, since it appears that all of the cells within the recipients’ bodies are showing marked improvement.
In some countries, there is already a legal market for blood plasma. In the wake of the BSE crisis of the 1990s, plasma donations are not used in the UK. But in the US, donors can make $200 a month (plus loyalty points) from plasma donations. The fresh plasma is separated from the blood, and the red blood cells returned to the bloodstream, in a sitting that lasts 90 minutes. The plasma is used in medical procedures, to treat coagulation disorders and immune deficiencies. The business is completely legitimate, but if young blood rejuvenates our cells is proved to have anti-ageing effects, the risk of backstreet operators setting up will soar. When I asked Wyss-Coray if the prospect worried him, he looked serious. “Absolutely,” he said. “There are always going to be nutcases.”
These are worst-case scenarios. The Stanford trial may find that simply injecting young plasma into old people has little or no effect. Wyss-Coray confesses that he suspects as much. He believes that rejuvenating older people might take a more potent brew than natural plasma. He has in mind a concentrated blend of 10 or 20 pro-youthful factors from young blood, mixed with antibodies that neutralise the effects of ageing factors found in old blood.
“As we get older, we have fewer stem cells and newly born neurons in our brains, and our learning and memory are affected,” says Villeda. “It’s not ddementia it’s just the natural degeneration associated with age.”
Amy Wagers emphasizes that no one has convincingly shown that young blood lengthens lives, and there is no promise that it will. Still, she says that young blood, or factors from it, may hold promise for helping elderly people to heal after surgery, or treating diseases of ageing.
Young mice blood has been studied to cause repair of age related damage such as cardiac hypertrophy, muscle dysfunction, demyelination processes and brain vasculature system in old mice. The mouse is the most common model organism for preclinical studies even though it has not proven particularly reliable at predicting the outcome of studies in humans.
Wyss-Coray one of the authors of the study mentioned in the question is a part of board of directors of a biotechnology start-up named Alkahest to explore the therapeutic implications of the mice findings in humans. The young mice blood treatment has been shown to have effects in old mice neural dysfunctions such as
1. Cardiac hypertrophy: Loffredo et.al. have concluded that treatment of old mice to restore GDF11 to youthful levels recapitulated the effects of parabiosis and reversed age-related hypertrophy, revealing a therapeutic opportunity for cardiac aging in 2013.
2. Muscle dysfunction: GDF11 systemically regulates muscle aging and may be therapeutically useful for reversing age-related skeletal muscle and stem cell dysfunction per conclusions of Sinha M et.al. in 2014.
3. Reversal of demyelination processes: Ruckh JM et.al. in 2012 concluded that enhanced remyelinating (Remyelination is a term for the re-generation of the nerve’s myelin sheath, damaged in many diseases) activity requires both youthful monocytes and other factors, and that remyelination-enhancing therapies targeting endogenous cells can be effective throughout life.
4. Improvement of brain vasculature system: Katsimpardi L et.al. in 2014 concluded that GDF11 alone can improve the cerebral vasculature and enhance neurogenesis. Studies in mice and Xenopus suggest that this protein is involved in mesodermal formation and neurogenesis during embryonic development. Research shows that there could be multiple forms of GDF11
Sources:
http://www.nature.com/news/ageing-research-blood-to-blood-1.16762
http://glennlaboratories.stanford.edu/
http://www.nature.com/news/blood-hormone-restores-youthful-hearts-to-old-mice-1.12971
http://www.bizjournals.com/sanfrancisco/print-edition/2014/01/31/conboy-uc-berkeley-aging-research.html
http://www.bizjournals.com/sanfrancisco/blog/biotech/2014/05/young-blood-stanford-researchers-hope-plasma.html
http://www.bizjournals.com/sanfrancisco/print-edition/2014/01/31/aging-calico-levinson-buck-institute.html
https://www.ucsf.edu/news/2014/01/122211/blood-work-scientists-uncover-surprising-new-tools-rejuvenate-brain
https://www.newscientist.com/article/mg22329831-400-young-blood-to-be-used-in-ultimate-rejuvenation-trial/
http://www.theguardian.com/science/2015/aug/04/can-we-reverse-ageing-process-young-blood-older-people
Inject-able Brain Implant Mapping

A simple inject-able brain implant is now all it takes to wire up a brain’s neurons. A diverse team of physicists, neuroscientists and chemists has implanted mouse brains with a rolled-up, silky mesh studded with tiny electronic devices, and shown that it unfurls to spy on and stimulate individual neurons.
The inject-able brain implant has the potential to unravel the workings of the mammalian brain in unprecedented detail. “I think it’s great, a very creative new approach to the problem of recording from large number of neurons in the brain,” says Rafael Yuste, director of the Neurotechnology Center at Columbia University in New York, who was not involved in the work.
If eventually shown to be safe, the soft mesh might even be used in humans as an inject-able brain implant to treat conditions such as Parkinson’s disease, concussions and issues arising from Traumatic Brain Injuries, says Charles Lieber, a chemist at Harvard University on Cambridge, Massachusetts, who led the team. The work was published in Nature Nanotechnology on 8 June.
How brain Cells Translate
Neuroscientists still do not understand how the activities of individual brain cells translate to higher cognitive powers such as perception and emotion. The problem has spurred a hunt for technologies that will allow scientists to study thousands, or ideally millions, of neurons at once, but the use of brain implants is currently limited by several disadvantages. So far, even the best technologies have been composed of relatively rigid electronics that act like sandpaper on delicate neurons. They also struggle to track the same neuron over a long period, because individual cells move when an animal breathes or its heart beats.
The Harvard team solved these problems by using a mesh of conductive polymer threads with either nano-scale electrodes or transistors attached at their intersections. Each strand is as soft as silk and as flexible as brain tissue itself. Free space makes up 95% of the mesh, allowing cells to arrange themselves around the inject-able brain implant.
In 2012, the team showed 22 that living cells grown in a dish can be coaxed to grow around these flexible scaffolds and meld with them, but this ‘cyborg’ tissue was created outside a living body. “The problem is, how do you get that into an existing brain?” says Lieber.
The team’s answer was to tightly roll up a 2D mesh a few centimeters wide and then use a needle just 100 micrometers in diameter to inject it directly into a target region through a hole in the top of the skull. The inject-able brain implant mesh unrolls to fill any small cavities and mingles with the tissue (see ‘Bugging the brain’). Nano-wires that poke out can be connected to a computer to take recordings and stimulate cells.
The Injectable Brain Implant
So far, the researchers have utilized the injectable brain implanted meshes consisting of 16 electrical elements into two brain regions of anesthetized mice, where they were able to both monitor and stimulate individual neurons. The mesh integrates tightly with the neural cells, says Jia Liu, a member of the Harvard team, with no signs of an elevated immune response after five weeks. Neurons “look at this polymer network as friendly, like a scaffold”, he says.
The next steps will be to implant larger meshes containing hundreds of devices, with different kinds of sensors, and to record activity in mice that are awake, either by fixing their heads in place, or by developing wireless technologies that would record from neurons as the animals moved freely. The team would also like to inject the device into the brains of newborn mice, where it would unfold further as the brain grew, and to add hairpin-shaped nano-wire probes to the mesh to record electrical activity inside and outside cells.
2014 Conference
When Lieber presented the work at a conference in 2014, it “left a few of us with our jaws dropping”, says Yuste.
There is huge potential for techniques that can study the activity of large numbers of neurons for a long period of time with only minimal damage, says Jens Schouenborg, head of the Neuronano Research Centre at Lund University in Sweden, who has developed a gelatin-based ‘needle’ for delivering electrodes to the brain. But he remains skeptical of this technique: “I would like to see more evidence of the inject-able brain implant’s long-term compatibility with the body,” he says. Rigorous testing would be needed before such a device could be implanted in people. But, says Lieber, it could potentially treat brain damage caused by a stroke, as well as Parkinson’s disease.
Lieber’s team is not funded by the US government’s US$4.5-billion Brain Research through Advancing Innovative Neurotechnologies (BRAIN) initiative, launched in 2013, but the work points to the power of that effort’s multidisciplinary approach, says Yuste, who was an early proponent of the BRAIN initiative. Bringing physical scientists into neuroscience, he says, could help to “break through the major experimental and theoretical challenges that we have to conquer in order to understand how the brain works”.
Source :
http://www.nature.com/news/injectable-brain-implant-spies-on-individual-neurons-1.17713?WT.ec_id=NATURE-20150611#b2
http://www.nature.com/news/neuroscience-tuning-the-brain-1.14900
http://www.nature.com/news/nih-serves-up-wide-menu-for-us-brain-mapping-initiative-1.13745
http://www.nature.com/news/ambitious-plans-for-brain-project-unveiled-1.15375
Home Safety To Prevent, Adapt and Decrease Hazards

As a caregiver, we need to be aware of hazards that cause falls, fractures, burns, and other accidents in the home. These incidents cause injury and loss of mobility for individuals who are challenged with vision, balance and coordination impairments. In addition to the pain and expense of the injury, many times depression, social isolation and a feeling of helplessness replace independence.
Some accidents can he caused by medical issues such as sharp drops in blood pressure, numbness in the legs or feet, certain sedatives or anti-depressants, or problems with balance and equilibrium. These problems should be discussed with the individual’s physician as soon as possible. Use this checklist to help make simple changes to make the home safer.
Many accidents can be prevented by thoroughly evaluating the safety of the home and making the necessary modifications. As the old saying goes, “An ounce of prevention is worth a pound of cure”. Take a close look at each entrance, room and stairwell. Check for hazards by using this checklist and then make the needed adaptations to provide a safe environment. By minimizing hazards, you are maximizing independence.
Preventing Falls
- Have clutter, newspapers, magazines or other objects been removed from the floor, stairs and counter-tops?
- Is there at least one sturdy, easy to grip handrail at the stairway? (Two are recommended if the individuals is utilizing a cane.)
- Have all rugs been secured with non-slip pads or tape?
- Does the individual wear sturdy, well fitting shoes? (Loose fitting and/or slip-on foot wear can cause an individual to be unstable when walking)
- Are there tripping hazards like electrical cords, footstools or other clutter near the floor, which might be difficult to see?
- Are lamps and appliances located near the outlets, so extension cords are not needed?
- Is the furniture placed with sufficient space allocated for easy egress around the room?
- Are the pots, pan and all the cooking utensils placed at a comfortable height?
- Is there a “Reaching Devise” available to utilize when selecting difficult to reach items in cabinets and on shelves?
- If a stepladder must be used, is it sturdy with handles and textured steps?
- Is there a sturdy cane, crutch, walker or bar close to the bed and chairs to assist in getting up?
- Can personal items such as eyeglasses, tissues, TV remotes or telephones easily be reached while in bed or sitting in a chair?
- Are light switches easily accessible?
- Have you considered changing the standard toggle switch to a rocker switch to help with ease of operating?
- Is the toilet at a comfortable height? (Consider adding a raised toilet seat, a toilet safety frame with armrests, or an over toilet adjustable commode)
- Are there grab bars near the toilet and tub and/or shower area? TOWEL BARS SHOULD NEVER BE USED AS HANDRAILS.
- Is there a bath chair in the shower area?
- Does the individual need a transfer tub bench to get in or out of the bathtub?
- Is there a hand-held shower spray that can be used while sitting on a bath chair or bench?
- Are necessary bath items (towels, washcloths, soap, shampoo, etc.) stored in an easy to reach location?
- Are towel bars, toilet and sink fixtures securely attached?
- Does the bathtub and/or shower have a non-slip surface?
- Are the knobs in the sink and tub clearly labeled. as hot and cold?
(If necessary, mark the hot water knob with red nail polish as a
reminder.) - Are the thermostat, electrical outlets and light switches at easily reached heights?
- Are outdoor steps kept sturdy and textured to prevent slipping? (Add tread strips to provide texture)
Lighting
Adequate lighting is essential throughout the home for safety and ‘Ay of life As individuals grow older, vision diminishes because …eyes restrict the amount of light that is coming in and is being absorbed. Frustration is common as simple tasks become more fi(&t because of vision changes. Make sure that regular eye exams j eyeglass prescriptions are kept up to date You can also help by making some modifications within the home.
- Is the lighting uniform from one room to the other? (Older eyes t ‘ke longer to adjust to light levels)
- Have you increased natural lighting by checking to see if windows and screens are clean?
- Is the lighting glare free? (eyes become more sensitive to glare as they age)
- Are all rooms hallways stairwells and entrances well lit?
- Are night -lights used in the bedrooms and bathrooms? (Motion activated lights do not interfere with sleeping.)
- Is there a motion activated light at the entranceway?
- If the threshold is at a different level it is adequately lit?
- Is lighting adequate for reading, sewing hobbies etc”
- Are there light switches at the top and bottom of staircases?
- Is there a plug-in rechargeable flashlight near each bed?
- Have wattages of bulbs been increased in lamps and fixtures to compensate for loss of vision? (Caution do not exceed ‘ianufactures posted guidelines)
Other Safety Concerns
Everyday safety practices and emergency planning cannot be left to chance. Review the plans with the individual periodically and practice emergency evacuations.
- Are emergency phone numbers AND the address of the residence posted near each telephone?
- Has everyone in the home been taught how to call 9-1-11 ● Is there an escape plan in case of fire?
- Is there a tornado or “shelterin place’ plan of action in place? ● Have all cords and wires been checked for fraying or wear?
- Is there a fire extinguisher readily available?
- Are smoke alarms and carbon monoxide alarms installed near each bedroom and the kitchen?
- Are batteries checked and changed when needed in smoke and carbon monoxide alarms monthly? Have non-working alarms been replaced?
- Are outlets and plugs warm? If so, avoid using until an electrician can check them.
- Are electrical outlets overloaded with cords? (Never have more
than one high-wattage appliance plugged into a single outlet.) - Avoid space heaters if possible. If they must be used, make sure
that they are kept away from flammable materials. - Is water temperature set at 120 degrees or less to prevent burns?
- Are flammable liquids stored away from heat sources?
- Are hot and cold-water knobs marked clearly? (Label the hot water knob with nail polish or paint, if necessary.)
- Can doorknobs be opened by the individual? (Consider changing knobs to levers that are easier to open.)
- Can the individual lock and unlock the door?
This guide nformation originated from the United Cerebral Palsy of Greater Birmingham
DeepMind – Google’s Human-Level Mind Control

Does DeepMind represent the initial step in software development becoming a major assist or replacement for controlling bodily functions in individual with Traumatic Brain and/or Spinal Cord injuries? Imagine a person suffering from one of those afflictions utilizing software to control the muscle functions of their body as they go about their normal everyday activities.
DeepMind, the Google-owned artificial-intelligence company, has revealed how it created a single computer algorithm that can learn how to play 49 different arcade games, including the 1970’s classics Pong and Space Invaders. In more than half of those games, the computer became skilled enough to beat a professional human player.
The algorithm — which has generated a buzz since publication of a preliminary version in 2013 (V. Mnih et al. Preprint at http://arxiv.org/abs/1312.5602; 2013) — is the first artificial-intelligence (AI) system that can learn a variety of tasks from scratch given only the same, minimal starting information. “The fact that you have one system that can learn several games, without any tweaking from game to game, is surprising and pretty impressive,” says Nathan Sprague, a machine-learning scientist at James Madison University in Harrisonburg, Virginia.
DeepMind, which is based in London, says that the brain-inspired system could also provide insights into human intelligence. “Neuroscientists are studying intelligence and decision-making, and here’s a very clean test bed for those ideas,” says Demis Hassabis, co-founder of DeepMind. He and his colleagues describe the gaming algorithm in a paper published this week
Games are to AI researchers what fruit flies are to biology — a stripped-back system in which to test theories, says Richard Sutton, a computer scientist who studies reinforcement learning at the University of Alberta in Edmonton, Canada. “Understanding the mind is an incredibly difficult problem, but games allow you to break it down into parts that you can study,” he says. But so far, most human-beating computers — such as IBM’s Deep Blue, which beat chess world champion Garry Kasparov in 1997, and the recently unveiled algorithm that plays Texas Hold ’Em poker essentially perfectly.
DeepMind’s versatility comes from joining two types of machine learning— an achievement that Sutton calls “a big deal”. The first, called deep learning, uses a brain-inspired architecture in which connections between layers of simulated neurons are strengthened on the basis of experience. Deep-learning systems can then draw complex information from reams of unstructured data (seeNature 505, 146–148; 2014). Google, of Mountain View, California, uses such algorithms to automatically classify photographs and aims to use them for machine translation.
The second is reinforcement learning, a decision-making system inspired by the neurotransmitter dopamine reward system in the animal brain. Using only the screen’s pixels and game score as input, the algorithm learned by trial and error which actions — such as go left, go right or fire — to take at any given time to bring the greatest rewards. After spending several hours on each game, it mastered a range of arcade classics, including car racing, boxing and Space Invaders.
This rapid growth of data sets means that machine learning can now use complex model classes and tackle highly non-trivial inference problems. Our human brain constantly solves non-trivial problems as we conduct our daily activities. Interpreting high-dimensional sensory data to determine how best to control all of the muscles in our body, including the functioning of our internal organs. The development of cutting edge software, like DeepMind, could assist and resolve many of the issues confronting Traumatic Brain and Spinal Cord Injury patients, beginning with recovering the ability to move their arms and legs.
Spinal Cord Regenerated With Nasal Cell Transplant

The spinal cord regenerated with nasal cells was pioneered by Prof. Geoffrey Raisman, who first identified their potential to repair nerve damage in mice. The olfactory en-sheathing cell transplantation has been successfully used to enable Darek Fidyka, who was paralyzed from the chest down in a knife attack in 2010, to walk again.
The future for cell regeneration is extremely vast according to Professor Geoffrey Raisman, who began experimenting with mice in this field with his first transplant in 1972, over 40 years ago. In years to come, utilizing his team’s first successful human regenerative cell transplant, as an initial first step, we will see strides made in stroke, heart and brain damage patients. The horizon is vast for the improvement of humanities health and well being.
http://youtu.be/OMJLg5K40U0
The paper reporting the transplant, which was carried out by surgeons in Poland and led by Geoffrey Raisman of the UCL Institute of Neurology, is published today in the journal Cell Transplantation (5). The technique involves taking specialized cells known as olfactory ensheathing cells (OECs) from the patient’s own patient’s olfactory bulbs, and then grafting these cells at the site of injury, where they promote nerve cell growth to bridge the gap and restore function. An added advantage in using the patient’s own cells is that it avoids the problem of rejection by their immune system.

Darek Fidyka, 40, from Poland, said walking again – with the support of a frame – was “an incredible feeling”, adding: “When you can’t feel almost half your body, you are helpless, but when it starts coming back it’s like you were born again.”
Prof Geoffrey Raisman, chair of neural regeneration at University College London’s Institute of Neurology, led the UK research team. He said what had been achieved was “more impressive than man walking on the moon“.
The treatment used olfactory ensheathing cells (OECs) – specialist cells that form part of the sense of smell. OECs act as pathway cells that enable nerve fibres in the olfactory system to be continually renewed. In the first of two operations, surgeons removed one of the patient’s olfactory bulbs and grew the cells in culture.
Two weeks later they transplanted the OECs into the spinal cord, which had been cut through in the knife attack apart from a thin strip of scar tissue on the right. They had just a drop of material to work with – about 500,000 cells. About 100 micro-injections of OECs were made above and below the injury with four thin strips of nerve tissue were taken from the patient’s ankle and placed across an 8mm (0.3in) gap on the left side of the cord.
The scientists believe the OECs provided a pathway to enable fibres above and below the injury to reconnect, using the nerve grafts to bridge the gap in the cord.
BBC Interview by Fergus Walsh with UK research team
Traumatic Brain and Spinal Injury Patients, Walk Again

Traumatic brain and Spinal injury patients, who have been paraplegics in the past for the remainder of their lives, have new hope to walk again on the horizon.
There has been a lot of activity in brain-computer interfaces to help such people.
Another pioneering research group in this area is the laboratory of Miguel Nicolelis at Duke University Center for Neuroengineering. Nicolelis and colleagues have shown that a rhesus monkey in North Carolina could, using only its brain, control the walking patterns of a robot in Japan. In 2011, they got a monkey to move a virtual arm and feel sensations from it.
This team is leading the Walk Again Project, an international consortium of research centers dedicated to creating brain-computer interfaces to restore movement.
A 29-year-old paraplegic literally kicked off soccer’s World Cup competition in Brazil, using a mind-controlled exoskeleton that looks as if it came from the “Iron Man” movies.
The organizers of the international Walk Again Project said the symbolic soccer-ball kick was performed during the World Cup’s opening ceremonies in São Paulo’s Corinthians Arena by Juliano Pinto. He’s an athlete from Galea in Brazil’s São Paulo State who lost the use of his legs after a car accident in 2006.
Seven other paralyzed patients who volunteered to go through months of training for the task watched from the sidelines.
“We did it!!!!” the project’s leader, Duke University neuroscientist Miguel Nicolelis, tweeted. Nicolelis spearheaded a team of more than 150 scientists to create the exoskeleton — an effort that he says cost the Brazilian government $14 million over the past two years.
Was Pinto’s few seconds of fame worth the cost? Probably not, if we’re just talking about a kickoff that took a couple of seconds to complete. But the project’s researchers said the advances made in the course of the years-long effort — and the exposure given to the next generation of brain-controlled prosthetic — could be priceless.
“The World Cup demonstration is ceremonial, as we have only a moment to show a kick,” Sanjay Joshi, a roboticist from the University of California at Davis who was involved in the Walk Again Project, told NBC News via email from Brazil. “But maybe that kick will inspire a child somewhere in the world to become a doctor, engineer or scientist.”
Joshi said the project’s long-term aim is to bring together neuroscience, engineering and medicine to build brain-controlled devices that can change the lives of paralyzed patients. Nicolelis struck a similar tone in a post-kickoff statement: “It is only the beginning of a future in which people with paralysis will be able to leave the wheelchair and literally walk again.”
How it works
The system blends the hardware of a battery-powered “Iron Man” exoskeleton with a control system that’s guided by brain waves. Pinto wore an electroencephalogram (EEG) cap dotted with electrodes, which picked up and magnified the faint electrical signals emanating through his skull. Sensors were built into the suit to detect muscle movements.
At first, Nicolelis considered using brain implants to control the suit, but he and his colleagues quickly determined that the EEG cap was less intrusive and more manageable.
During the training period, Pinto and the seven other subjects learned to think about moving their feet in such a way that the corresponding signals from their brains and muscles would register with the computerized guidance system. The exosuit’s wearer received feedback from the feet in the form of buzzing vibrations felt on the skin.
All eight patients learned to walk using the suit, and one overachiever took “a total of 132 steps, to the awe of everyone present,” Nicolelis told NBC News.
At the World Cup ceremonies, all it took was a tap from Pinto’s robo-leg to send the soccer ball rolling. Meanwhile, assistants stood on either side, helping to steady the bulky suit. The moment passed so quickly that many TV viewers missed it.
What it means
In the wake of the World Cup kickoff, experts who weren’t involved in the Walk Again Project debated whether the effort scored a winning goal.
“The demo did not advance the state of the art,” Jose Contreras-Vidal, a biomedical engineer at the University of Houston, told NBC News in an email. “Certainly our NeuroRex was the first and remains the only brain-controlled exoskeleton to allow spinal cord injury patients to walk over-ground unassisted, and we have been able to do so with about 10 percent of the funding Dr. Nicolelis has received to develop their exo.”
Contreras-Vidal said one of the metrics for evaluating the return on investment should be the number of Brazilian scientists and students who benefit from their involvement in the Walk Again Project.
“I suppose the infrastructure will remain in Brazil, which is good,” Contreras-Vidal wrote. “What matters now is what the plans are for the future. Clinical (longitudinal) trials must be done with patients, once the system is completed and validated. Dr. Nicolelis is not known for working with EEG and walking robotics, and thus expertise in these areas would need to be developed and retained in Brazil to continue the project. We hope he succeeds.”
Anil Raj, a research scientist at the Florida Institute for Human and Machine Cognition, agreed that the project’s real value depends on what comes after the kick.
“A successful kick is a demonstration event, but the technological development needed to be able to attempt the demo is the contribution to the future of exoskeletons for those with spinal cord injury,” Raj said in an email. “$14 million for training eight patients and building a novel exoskeleton and brain-controlled interface seems to me to be a reasonable expenditure.”

